Opioid Epidemic Ignores Boundaries in North Carolina
The opioid epidemic in North Carolina ignores boundaries and divisions, plaguing rural, urban, and suburban communities alike.
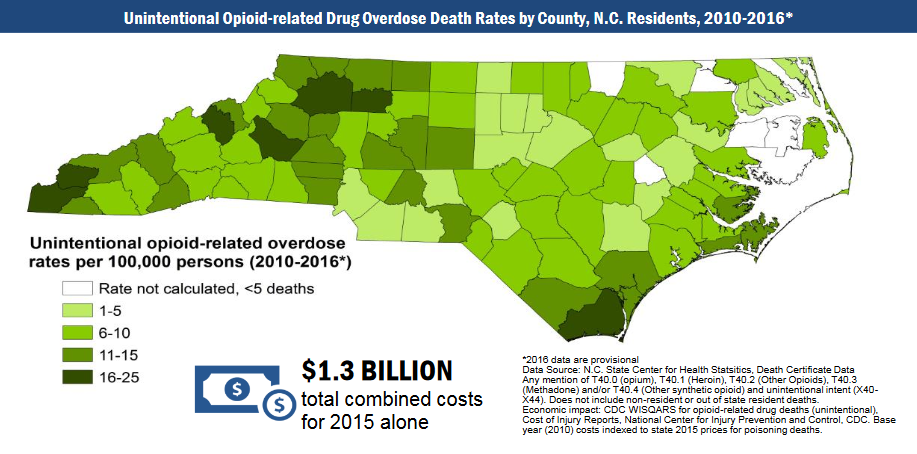
At its recent NC Rural Assembly titled “Claiming Our Future,” the NC Rural Center offered an important discussion on the opioid epidemic in North Carolina. Introduced by Dr. Anu Rao-Patel from Blue Cross Blue Shield of NC, the session began with sobering statistics — including the fact that drug overdoses are now the leading cause of accidental death in NC (ahead of vehicular crashes). According to Centers for Disease Control and Prevention estimates, the cost of unintentional opioid related overdose deaths in NC totaled $1.3 billion in 2015.
The opioid epidemic in North Carolina ignores boundaries and divisions, plaguing rural, urban, and suburban communities alike. Steve Mange from the NC Department of Justice advised that the state must pursue prevention, treatment and recovery, and enforcement against drug traffickers. He also described impacts of the epidemic, including:
- Increasing healthcare costs,
- Rising criminal justice costs,
- Declining workforce participation, and
- Increasing demand for social services.
Mange echoed the comments of Attorney General Josh Stein at the “Roundtable on the Economic Aspects of the Opioid Crisis” hosted by the Kenan Institute for Private Enterprise in October: “Sheriffs are telling me that 70 to 80 percent of the people in their jails are there because they committed a drug crime … or they engaged in a property crime to feed their addiction.” Stein went on to say that “jail is not a cost-effective way to deal with addiction.”
Speaking at last month’s Rural Assembly, Allan Dellapenna from the NC Division of Public Health agreed with Attorney General Stein and indicated that treatment for addiction costs less than incarceration. He presented the NC Opioid Action Plan, which states: “To tackle this health crisis, the N.C. Department of Health and Human Services is working to connect people with preventative healthcare, substance use disorder treatment, and community supports.” The plan involves strategies the state and its partners will pursue in an effort to reduce opioid overdose deaths by 20 percent by 2021. Resources such as data on Opioid and Heroin Poisoning Deaths, Emergency Department Visits, and Hospitalizations by County are also available from the plan.

Secretary Mandy Cohen and Dr. Susan Kansagra from the NC Department of Health & Human Services presented an update on the opioid action plan and implementation of the 2017 STOP Act (effective Jan. 1, 2018) to the Joint Legislative Committee on Health and Human Services in November. NC House Speaker Tim Moore recently appointed Rep. Greg Murphy, MD, a Greenville physician and chief sponsor of the STOP Act, to lead a task force on opioid sentencing reform, as reported in the Greenville Daily Reflector. At the Kenan Institute roundtable, Rep. Murphy stated, “We’re not treating the people that we need to treat. These aren’t bad people. These are people who have an addiction problem, but it’s a chemical problem.” Steve Mange shared at the Rural Assembly that only one in ten individuals with substance-abuse issues receive proper treatment. However, he also indicated progress made in reversing overdoses with naloxone — last year there were more overdose reversals than accidental deaths in North Carolina.

The opioid epidemic has negative implications for the state’s workforce as well. For more on labor force participation implications by county, see economist Alan Krueger’s work published by the Brookings Institution. Krueger found that labor force participation rates for men and women declined more in counties where more opioids were prescribed by medical personnel. These findings are particularly significant for the counties shaded in green with large black circles (indicating the highest amounts of opioid prescriptions dispensed per person) in the second map that appears above.

According to Castlight Health, four NC municipalities rank among the top 25 worst cities in the United States for opioid abuse: Wilmington (#1), Hickory (#5), Jacksonville (#12), and Fayetteville (#18). The final presenter at the Rural Assembly was Jamie Treadway, who represented the Catawba Valley Community Foundation from the Hickory region. He described the foundation’s efforts to respond to the epidemic in their community, which include sponsoring substance abuse training for local teachers and counselors in March 2018.
The opioid epidemic presents many challenges for communities in North Carolina. It is a complex problem that will require state and local stakeholders to work together in pursuit of solutions, whether they reside in rural, urban, or suburban communities. ncIMPACT and the UNC School of Government are dedicated to assisting them with this important work.


