Targeted Universalism Uses Social Capital to Increase Equity in COVID-19 Recovery
By practicing targeted universalism, policymakers can aim specific strategies, such as social capital-based programming, at problems that plague marginalized groups to advance equity in COVID-19 economic recovery efforts.

The Problem
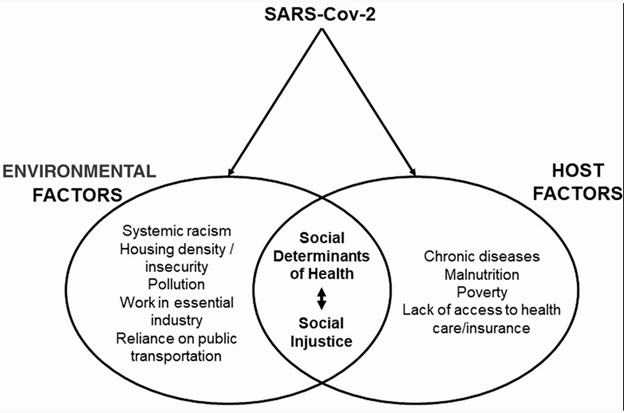
Data shows that certain social determinants prevalent in vulnerable communities are also associated with greater negative impacts from COVID-19. Some examples include chronic medical conditions, low healthcare access, poverty, frontline work, poor living conditions, communication gaps, and inadequate transportation.
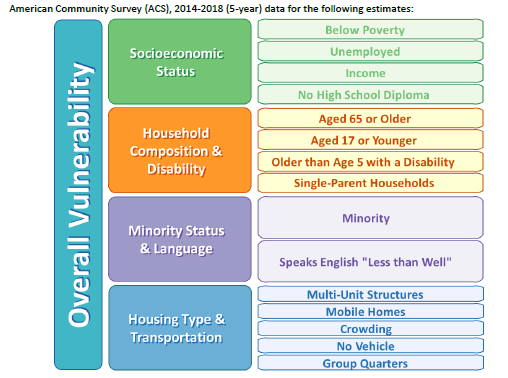
The Centers for Disease Control (CDC) offer a useful model called the Social Vulnerability Index (SVI) for gauging each community’s vulnerability. There are 15 factors in the SVI, grouped into four categories: socioeconomic status, household composition/disability, minority status/language, and housing/transportation. Communities with a higher social vulnerability index tend to experience greater negative impacts from disasters, and the trend has held for the COVID-19 pandemic.
Examining social determinants is important because of their propensity to manifest as biomedical factors that can increase the urgency for persons experiencing disasters, especially medical disasters like the pandemic. For COVID-19 patients, chronic medical conditions such as diabetes, obesity, and heart disease have been the primary biomedical factors contributing to greater negative outcomes from the virus. Within minority groups, the prevalence of chronic medical conditions is greater than in other groups. As a result, minority groups have experienced hospitalization and death more than others in the United States. The challenge for public administrators is to find ways to mitigate the biomedical factors that act as comorbidities. Given that the prevalence of chronic medical conditions in minority communities is due to many contributing causes, public administrators can use the method of targeted universalism to isolate some of these causes and develop public programming that seeks to improve outcomes in specific areas.
Social Vulnerability Index (SVI) – Centers for Disease Control
The Response
As a result of the disproportionate effects the pandemic had on disadvantaged communities, in its U.S. COVID-19 Global Response and Recovery Framework (2021), the White House listed equity as one of its cross-cutting principles, encouraging public administrators to develop programming to mitigate the underlying causes of inequity. By developing specific strategies to mitigate the social determinants that are prevalent within vulnerable communities and that acted as comorbidities during the pandemic, public administrators can work to promote equity for marginalized communities. Many social determinants that contributed to the disproportionate impact of COVID-19 have a direct association with social capital. One of the most influential determinants of the pandemic’s impact was the access to resources within each community. For example, access to healthcare, information, transportation, and financial capital positively correlates with COVID-19 outcomes.
When considering the different social determinants that have influenced COVID-19 outcomes, a few come to mind that seem to have an inherent relationship with a given individual’s social network structures. Two related examples are profession and financial capacity. Financial resources are one of the most significant resources an individual can have due to their capacity to connect that individual to many other resources. For example, middle- and high-income individuals tend to have much more developed social networks than low-income individuals, who are more likely to rely on family when in need. Simultaneously, many social determinants that resulted in the disproportionate impact of the virus were collective characteristics of entire communities, e.g., lower access to healthcare, gaps in healthcare communication, and living conditions. As public administrators seek to develop social capital-based programming to mitigate social determinants, it could be beneficial to develop a two-pronged approach to targeted universalism that considers individual and collective social determinants separately.
COVID-19 DISPARITIES THROUGH SOCIAL DETERMINANTS OF HEALTH LENS
Clinical Infectious Diseases, Volume 72, Issue 4, 15 February 2021, Pages 703–706
The Players
Looking at individual social determinants, social capital-based programming that seeks to improve professional and financial opportunities for individuals in vulnerable communities can help drive equity as an outcome of COVID-19 recovery in the United States. Expanding job opportunities for individuals in vulnerable communities will mandate their development of the ability to generate linking social capital. There is evidence that an individual’s social network structure significantly influences her job opportunities. Social capital-based programming that seeks to help disadvantaged persons build the social and professional skills they need to be successful could help to mitigate this social determinant by offering participants opportunities to build linking social capital, enabling them to connect and engage with individuals who occupy more senior positions in professional hierarchies.
In examining collective social determinants, the biomedical comorbidities prevalent in disadvantaged communities and low access to healthcare worsened outcomes significantly. Individuals suffering from preexisting conditions more often needed ventilators and intensive care, yet they were sent to hospitals running short of these resources. Mitigating the low healthcare access in vulnerable communities via social capital-based programming might be most effective when it seeks to empower communities via collaboration, resource-sharing, and support to break down barriers. In practice, it might mean collaborating with nonprofits that offer translation services to improve hospital care for minorities. It could mean designing a billing structure that would allow the funneling of critical care patients to private healthcare providers with available resources. Employing community healthcare workers to guide community members toward resources could also help mitigate the problem.
An individual’s social network structure significantly influences her job opportunities.
The Promise
To advance equity as an outcome of COVID-19 recovery efforts in the United States, it will be important to develop an approach that mitigates the symptoms of inequity and the underlying causes. Many of these causes are social determinants that have direct relationships with social capital at both the individual and community-wide levels. By pursuing a two-pronged version of targeted universalism, public administrators can make lasting changes in communities by helping individuals to change the structures of their social networks, thus opening the door to better opportunities, and by helping communities to gain access to resources that would better situate them to protect the members of their constituencies from the effects of any disaster.